BigData@Heart Papers
Association between beta-blocker use and mortality/morbidity in older patients with heart failure with reduced ejection fraction. A propensity score-matched analysis from the Swedish Heart Failure Registry.
Published: 3 September 2019, European Journal of Heart Failure
Authors: Stolfo D, Uijl A, Schrage B, Fudim M, Asselbergs FW, Koudstaal S, Sinagra G, Dahlstrom U, Rosano G, and Savarese G
Abstract
Background
Beta‐blockers reduce mortality and morbidity in heart failure with reduced ejection fraction (HFrEF). However, patients older than 80 years are poorly represented in randomized controlled trials (RCTs). We assessed the association between beta‐blocker use and outcomes in HFrEF patients ≥80 years.
Methods and results
We included patients with EF<40%, age ≥80 years from the Swedish HF Registry. The association between beta‐blocker use, all‐cause mortality and cardiovascular (CV) mortality/HF hospitalization was assessed by Cox proportional hazard models in a 1:1 propensity score (PS)‐matched cohort. To assess consistency, the same analyses were performed in a positive control cohort with age <80 years. A negative control outcome analysis was run using hospitalization for cancer as endpoint.
Of 6,562 patients aged ≥80 years, 5640 (86%) received beta‐blockers. In the matched cohort including 1,732 patients, beta‐blocker use was associated with a significant reduction in risk of all‐cause mortality (HR: 0.89; 95%CI: 0.79–0.99). Reduction in CV mortality/HF hospitalization was not significant (HR: 0.94; 95%CI: 0.85–1.05) due to the lack of association with HF hospitalization, whereas CV death was significantly reduced. After adjustment rather than matching for the PS in the overall cohort, beta‐blocker use was associated with reduced risk of all outcomes. In patients aged <80 years, use of beta‐blockers was associated with reduced risk of all‐cause death (HR: 0.79, 95%CI: 0.68‐0.92) and of the composite outcome (HR: 0.88, 95%CI: 0.77‐0.99).
Conclusions
In HFrEF patients ≥80 years of age, use of beta‐blockers was high and was associated with improved all‐cause and CV survival.
Read the full paper here: https://onlinelibrary.wiley.com/doi/abs/10.1002/ejhf.1615#.XW-Ews-iNzs.twitter
Association between use of primary prevention implantable cardioverter-defibrillators and mortality in patients with heart failure. A prospective propensity-score matched analysis from the Swedish heart failure registry.
Published: 3 September 2019, Circulation-Heart Failure
Authors: Schrage B, Uijl A, Benson L, Westermann D, Ståhlberg M, Stolfo D, Dahstrom U, Linde C, Braunschweig F, and Savarese G.
Background
Most randomized trials on implantable cardioverter-defibrillator (ICD) use for primary prevention of sudden cardiac death in heart failure with reduced ejection fraction (HFrEF) enrolled patients >20 years ago. We investigated the association between ICD use and all-cause mortality in a contemporary HFrEF cohort and examined relevant subgroups.
Methods
Patients from the Swedish HF Registry (SwedeHF) fulfilling the European Society of Cardiology criteria for primary prevention ICD were included. The association between ICD use and 1-year and 5-year all-cause and cardiovascular (CV) mortality was assessed by Cox Regression models in a 1:1 propensity score matched cohort and in prespecified subgroups.
Results
Of 16,702 eligible patients, only 1,599 (10%) had an ICD. After matching, 1,305 ICD recipients were compared to 1,305 non-recipients. ICD use was associated with a reduction in all-cause mortality risk within 1 year [hazard ratio (HR): 0.73, 95% confidence interval (CI): 0.60-0.90] and 5 years (HR: 0.88, 95%CI: 0.78-0.99). Results were consistent in all subgroups including patients with vs. without ischemic heart disease, males vs. females, in those aged <75 vs. ≥75 years, in those with earlier vs. later enrollment in SwedeHF and in patients with vs. without cardiac resynchronization therapy.
Conclusions
In a contemporary HFrEF population, ICD for primary prevention was underused although it was associated with reduced short- and long-term all-cause mortality. This association was consistent across all the investigated subgroups. These results call for better implementation of ICD therapy.
Read the full paper here: https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.119.043012
Sub-types of atrial fibrillation with concomitant valvular heart disease derived from electronic health records: phenotypes, population prevalence, trends and prognosis
Published: 13 August 2019, EP Europace
Authors: Banerjee A, Allan V, Denaxas S, Shah A, Kotecha D, Lambiase P D, Jacob J, Lund L H, Hemingway H
Abstract
Aims
To evaluate population-based electronic health record (EHR) definitions of atrial fibrillation (AF) and valvular heart disease (VHD) subtypes, time trends in prevalence and prognosis.
Methods and results
A total of 76 019 individuals with AF were identified in England in 1998–2010 in the CALIBER resource, linking primary and secondary care EHR. An algorithm was created, implemented, and refined to identify 18 VHD subtypes using 406 diagnosis, procedure, and prescription codes. Cox models were used to investigate associations with a composite endpoint of incident stroke (ischaemic, haemorrhagic, and unspecified), systemic embolism (SSE), and all-cause mortality. Among individuals with AF, the prevalence of AF with concomitant VHD increased from 11.4% (527/4613) in 1998 to 17.6% (7014/39 868) in 2010 and also in individuals aged over 65 years. Those with mechanical valves, mitral stenosis (MS), or aortic stenosis had highest risk of clinical events compared to AF patients with no VHD, in relative [hazard ratio (95% confidence interval): 1.13 (1.02–1.24), 1.20 (1.05–1.36), and 1.27 (1.19–1.37), respectively] and absolute (excess risk: 2.04, 4.20, and 6.37 per 100 person-years, respectively) terms. Of the 95.2% of individuals with indication for warfarin (men and women with CHA2DS2-VASc ≥1 and ≥2, respectively), only 21.8% had a prescription 90 days prior to the study.
Conclusion
Prevalence of VHD among individuals with AF increased from 1998 to 2010. Atrial fibrillation associated with aortic stenosis, MS, or mechanical valves (compared to AF without VHD) was associated with an excess absolute risk of stroke, SSE, and mortality, but anticoagulation was underused in the pre-direct oral anticoagulant (DOAC) era, highlighting need for urgent clarity regarding DOACs in AF and concomitant VHD.
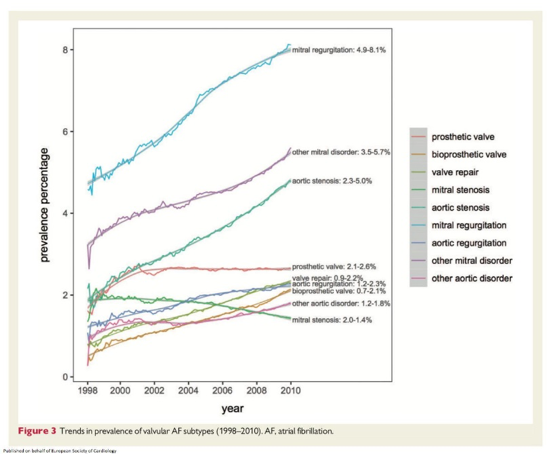
Read the full paper here: https://doi.org/10.1093/europace/euz220
Two preprint articles on BioRxiv
- Genome-wide association study provides new insights into the genetic architecture and pathogenesis of heart failure
- Genetic determinants of lipids and cardiovascular disease outcomes: a wide-angled Mendelian randomization investigation